HAEM5:Acute myeloid leukaemia with DEK::NUP214 fusion: Difference between revisions
| [checked revision] | [checked revision] |
No edit summary |
No edit summary |
||
| Line 75: | Line 75: | ||
|D, P | |D, P | ||
|Yes (WHO) | |Yes (WHO) | ||
|The t(6;9) occurs in 0.6-1.7% of AML cases in children (REFERENCES) and about 1% of adult AML cases (REFERENCES). ''DEK''::''NUP214'' has traditionally been associated with a poor prognosis in both adult and pediatric AML cases<ref name=":0" />. Of note, a 2014 retrospective analysis suggests a better outcome for pediatric patients with this translocation than previously reported<ref>{{Cite journal|last=Sandahl|first=Julie Damgaard|last2=Coenen|first2=Eva A.|last3=Forestier|first3=Erik|last4=Harbott|first4=Jochen|last5=Johansson|first5=Bertil|last6=Kerndrup|first6=Gitte|last7=Adachi|first7=Souichi|last8=Auvrignon|first8=Anne|last9=Beverloo|first9=H. Berna|date=2014|title=t(6;9)(p22;q34)/DEK-NUP214-rearranged pediatric myeloid leukemia: an international study of 62 patients|url=https://www.ncbi.nlm.nih.gov/pubmed/24441146|journal=Haematologica|volume=99|issue=5|pages=865–872|doi=10.3324/haematol.2013.098517|issn=1592-8721|pmc=4008104|pmid=24441146}}</ref>. Elevated white blood cell counts and higher bone marrow blast percentages are associated with shorter periods of overall survival and disease-free survival, respectively<ref name=":0" />. Limited data suggests early allogeneic stem cell transplantation may be associated with better overall survival compared to patients without transplantation, suggesting accurate diagnosis for these patients is crucial<ref name=":0" /><ref>{{Cite journal|last=Slovak|first=M. L.|last2=Gundacker|first2=H.|last3=Bloomfield|first3=C. D.|last4=Dewald|first4=G.|last5=Appelbaum|first5=F. R.|last6=Larson|first6=R. A.|last7=Tallman|first7=M. S.|last8=Bennett|first8=J. M.|last9=Stirewalt|first9=D. L.|date=2006|title=A retrospective study of 69 patients with t(6;9)(p23;q34) AML emphasizes the need for a prospective, multicenter initiative for rare 'poor prognosis' myeloid malignancies|url=https://www.ncbi.nlm.nih.gov/pubmed/16628187|journal=Leukemia|volume=20|issue=7|pages=1295–1297|doi=10.1038/sj.leu.2404233|issn=0887-6924|pmid=16628187}}</ref><ref>{{Cite journal|last=Ishiyama|first=K.|last2=Takami|first2=A.|last3=Kanda|first3=Y.|last4=Nakao|first4=S.|last5=Hidaka|first5=M.|last6=Maeda|first6=T.|last7=Naoe|first7=T.|last8=Taniguchi|first8=S.|last9=Kawa|first9=K.|date=2012|title=Allogeneic hematopoietic stem cell transplantation for acute myeloid leukemia with t(6;9)(p23;q34) dramatically improves the patient prognosis: a matched-pair analysis|url=https://www.ncbi.nlm.nih.gov/pubmed/21869835|journal=Leukemia|volume=26|issue=3|pages=461–464|doi=10.1038/leu.2011.229|issn=1476-5551|pmid=21869835}}</ref>. The concurrent presence of FLT3-ITD does not appear to negatively impact survival in the pediatric population<ref name=":0" />. | | | ||
* The t(6;9) occurs in 0.6-1.7% of AML cases in children<ref name=":1" /> (REFERENCES) and about 1% of adult AML cases (REFERENCES). | |||
* ''DEK''::''NUP214'' has traditionally been associated with a poor prognosis in both adult and pediatric AML cases<ref name=":0" />. Of note, a 2014 retrospective analysis suggests a better outcome for pediatric patients with this translocation than previously reported<ref name=":1">{{Cite journal|last=Sandahl|first=Julie Damgaard|last2=Coenen|first2=Eva A.|last3=Forestier|first3=Erik|last4=Harbott|first4=Jochen|last5=Johansson|first5=Bertil|last6=Kerndrup|first6=Gitte|last7=Adachi|first7=Souichi|last8=Auvrignon|first8=Anne|last9=Beverloo|first9=H. Berna|date=2014|title=t(6;9)(p22;q34)/DEK-NUP214-rearranged pediatric myeloid leukemia: an international study of 62 patients|url=https://www.ncbi.nlm.nih.gov/pubmed/24441146|journal=Haematologica|volume=99|issue=5|pages=865–872|doi=10.3324/haematol.2013.098517|issn=1592-8721|pmc=4008104|pmid=24441146}}</ref>. Elevated white blood cell counts and higher bone marrow blast percentages are associated with shorter periods of overall survival and disease-free survival, respectively<ref name=":0" />. Limited data suggests early allogeneic stem cell transplantation may be associated with better overall survival compared to patients without transplantation, suggesting accurate diagnosis for these patients is crucial<ref name=":0" /><ref>{{Cite journal|last=Slovak|first=M. L.|last2=Gundacker|first2=H.|last3=Bloomfield|first3=C. D.|last4=Dewald|first4=G.|last5=Appelbaum|first5=F. R.|last6=Larson|first6=R. A.|last7=Tallman|first7=M. S.|last8=Bennett|first8=J. M.|last9=Stirewalt|first9=D. L.|date=2006|title=A retrospective study of 69 patients with t(6;9)(p23;q34) AML emphasizes the need for a prospective, multicenter initiative for rare 'poor prognosis' myeloid malignancies|url=https://www.ncbi.nlm.nih.gov/pubmed/16628187|journal=Leukemia|volume=20|issue=7|pages=1295–1297|doi=10.1038/sj.leu.2404233|issn=0887-6924|pmid=16628187}}</ref><ref>{{Cite journal|last=Ishiyama|first=K.|last2=Takami|first2=A.|last3=Kanda|first3=Y.|last4=Nakao|first4=S.|last5=Hidaka|first5=M.|last6=Maeda|first6=T.|last7=Naoe|first7=T.|last8=Taniguchi|first8=S.|last9=Kawa|first9=K.|date=2012|title=Allogeneic hematopoietic stem cell transplantation for acute myeloid leukemia with t(6;9)(p23;q34) dramatically improves the patient prognosis: a matched-pair analysis|url=https://www.ncbi.nlm.nih.gov/pubmed/21869835|journal=Leukemia|volume=26|issue=3|pages=461–464|doi=10.1038/leu.2011.229|issn=1476-5551|pmid=21869835}}</ref>. | |||
* The concurrent presence of FLT3-ITD does not appear to negatively impact survival in the pediatric population<ref name=":0" />. | |||
|} | |} | ||
==Individual Region Genomic Gain/Loss/LOH== | ==Individual Region Genomic Gain/Loss/LOH== | ||
| Line 132: | Line 135: | ||
|<span class="blue-text">EXAMPLE:</span> T | |<span class="blue-text">EXAMPLE:</span> T | ||
|<span class="blue-text">EXAMPLE:</span> Yes (NCCN) | |<span class="blue-text">EXAMPLE:</span> Yes (NCCN) | ||
|FLT3-ITD occurs in 69% of children and 78% of adults. In contrast to FLT3-ITD mutations, FLT3-TKD is very uncommon. The concurrent presence of FLT3-ITD with t(6;9) does not appear to negatively impact survival in the pediatric population<ref name=":0" />. | | | ||
* FLT3-ITD occurs in 69% of children and 78% of adults. | |||
* In contrast to FLT3-ITD mutations, FLT3-TKD is very uncommon. | |||
* The concurrent presence of FLT3-ITD with t(6;9) does not appear to negatively impact survival in the pediatric population<ref name=":0" />. | |||
|}Note: A more extensive list of mutations can be found in [https://www.cbioportal.org/ <u>cBioportal</u>], [https://cancer.sanger.ac.uk/cosmic <u>COSMIC</u>], and/or other databases. When applicable, gene-specific pages within the CCGA site directly link to pertinent external content. | |}Note: A more extensive list of mutations can be found in [https://www.cbioportal.org/ <u>cBioportal</u>], [https://cancer.sanger.ac.uk/cosmic <u>COSMIC</u>], and/or other databases. When applicable, gene-specific pages within the CCGA site directly link to pertinent external content. | ||
==Epigenomic Alterations== | ==Epigenomic Alterations== | ||
Revision as of 08:53, 17 May 2025
N/Haematolymphoid Tumours (WHO Classification, 5th ed.)
| This page is under construction |
editContent Update To WHO 5th Edition Classification Is In Process; Content Below is Based on WHO 4th Edition ClassificationThis page was converted to the new template on 2023-12-07. The original page can be found at HAEM4:Acute Myeloid Leukemia (AML) with t(6;9)(p23;q34.1); DEK-NUP214.
Primary Author(s)*
Jennelle C. Hodge, PhD, FACMG
WHO Classification of Disease
| Structure | Disease |
|---|---|
| Book | Haematolymphoid Tumours (5th ed.) |
| Category | Myeloid proliferations and neoplasms |
| Family | Acute myeloid leukaemia |
| Type | Acute myeloid leukaemia with defining genetic abnormalities |
| Subtype(s) | Acute myeloid leukaemia with DEK::NUP214 fusion |
WHO Essential and Desirable Genetic Diagnostic Criteria
| WHO Essential Criteria (Genetics)* | Presence of DEK::NUP214 fusion |
| WHO Desirable Criteria (Genetics)* | Detection of t(6;9)(p22.3;q34.1) |
| Other Classification | N/A |
*Note: These are only the genetic/genomic criteria. Additional diagnostic criteria can be found in the WHO Classification of Tumours.
Related Terminology
| Acceptable | |
| Not Recommended |
Gene Rearrangements
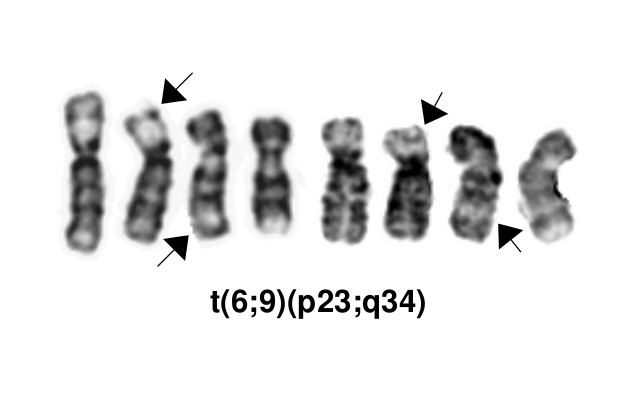
This AML subtype is classified based on the presence of a t(6;9)(p23;q34.1), which results in fusion of the 5’ portion of DEK at “6p23” (specifically 6p22.3[hg38]) and the 3’ portion of NUP214(CAN) at “9q34.1” (specifically 9q34.13[hg38])[1][2]. The breakpoints are intronic, producing an in-frame fusion[3]. The DEK-NUP214 fusion present on the derivative chromosome 6 is considered the pathogenic entity as the reciprocal NUP214-DEK fusion on chromosome 9 does not appear to be transcribed[4]. Typically, the DEK-NUP214 fusion presents as the sole abnormality but can be part of a complex karyotype[1]. Cases with the 6;9 translocation and <20% blasts are not currently classified as AML, which is controversial. Such cases should have close follow-up to monitor for development of more definitive evidence of AML or may be treated as AML if clinically appropriate[1].
| Driver Gene | Fusion(s) and Common Partner Genes | Molecular Pathogenesis | Typical Chromosomal Alteration(s) | Prevalence -Common >20%, Recurrent 5-20% or Rare <5% (Disease) | Diagnostic, Prognostic, and Therapeutic Significance - D, P, T | Established Clinical Significance Per Guidelines - Yes or No (Source) | Clinical Relevance Details/Other Notes |
|---|---|---|---|---|---|---|---|
| DEK | DEK::NUP214 | The pathogenic derivative is the der(6) resulting in fusion of the proto-oncogene 5’ DEK and 3’NUP214(CAN). | t(6;9)(p23;q34.1) | Rare (AML) | D, P | Yes (WHO) |
|
Individual Region Genomic Gain/Loss/LOH
| Chr # | Gain, Loss, Amp, LOH | Minimal Region Cytoband and/or Genomic Coordinates [Genome Build; Size] | Relevant Gene(s) | Diagnostic, Prognostic, and Therapeutic Significance - D, P, T | Established Clinical Significance Per Guidelines - Yes or No (Source) | Clinical Relevance Details/Other Notes |
|---|---|---|---|---|---|---|
| N/A |
Characteristic Chromosomal or Other Global Mutational Patterns
| Chromosomal Pattern | Molecular Pathogenesis | Prevalence -
Common >20%, Recurrent 5-20% or Rare <5% (Disease) |
Diagnostic, Prognostic, and Therapeutic Significance - D, P, T | Established Clinical Significance Per Guidelines - Yes or No (Source) | Clinical Relevance Details/Other Notes |
|---|---|---|---|---|---|
| N/A |
Gene Mutations (SNV/INDEL)
COSMIC does not have specific information on mutations related to this subtype of AML.
| Gene | Genetic Alteration | Tumor Suppressor Gene, Oncogene, Other | Prevalence -
Common >20%, Recurrent 5-20% or Rare <5% (Disease) |
Diagnostic, Prognostic, and Therapeutic Significance - D, P, T | Established Clinical Significance Per Guidelines - Yes or No (Source) | Clinical Relevance Details/Other Notes |
|---|---|---|---|---|---|---|
| FLT3
|
ITD mutations | Oncogene | Common (AML with DEK::NUP214 fusion) | EXAMPLE: T | EXAMPLE: Yes (NCCN) |
|
Note: A more extensive list of mutations can be found in cBioportal, COSMIC, and/or other databases. When applicable, gene-specific pages within the CCGA site directly link to pertinent external content.
Epigenomic Alterations
Not applicable
Genes and Main Pathways Involved
The molecular mechanism is not completely understood, but the fusion protein is known to act as an aberrant transcription factor, alter nuclear transport and induce myeloid cell-specific global protein synthesis[1][8].
| Gene; Genetic Alteration | Pathway | Pathophysiologic Outcome |
|---|---|---|
| N/A |
Genetic Diagnostic Testing Methods
Karyotype, FISH, RT-PCR
Familial Forms
Not applicable
Additional Information
Not applicable
Links
References
(use the "Cite" icon at the top of the page) (Instructions: Add each reference into the text above by clicking where you want to insert the reference, selecting the “Cite” icon at the top of the wiki page, and using the “Automatic” tab option to search by PMID to select the reference to insert. If a PMID is not available, such as for a book, please use the “Cite” icon, select “Manual” and then “Basic Form”, and include the entire reference. To insert the same reference again later in the page, select the “Cite” icon and “Re-use” to find the reference; DO NOT insert the same reference twice using the “Automatic” tab as it will be treated as two separate references. The reference list in this section will be automatically generated and sorted.)
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 WHO Classification of Tumours Editorial Board, eds, WHO Classification of Tumours, Haematolymphoid Tumours, 5th edition, IARC Press:Lyon, 2024. Online at: WHO Classification of Tumours.
- ↑ Khoury, Joseph D.; et al. (2022-07). "The 5th edition of the World Health Organization Classification of Haematolymphoid Tumours: Myeloid and Histiocytic/Dendritic Neoplasms". Leukemia. 36 (7): 1703–1719. doi:10.1038/s41375-022-01613-1. ISSN 1476-5551. PMC 9252913 Check
|pmc=value (help). PMID 35732831 Check|pmid=value (help). Check date values in:|date=(help) - ↑ von Lindern, M.; et al. (1992). "The translocation (6;9), associated with a specific subtype of acute myeloid leukemia, results in the fusion of two genes, dek and can, and the expression of a chimeric, leukemia-specific dek-can mRNA". Molecular and Cellular Biology. 12 (4): 1687–1697. doi:10.1128/mcb.12.4.1687. ISSN 0270-7306. PMC 369612. PMID 1549122.CS1 maint: PMC format (link)
- ↑ von Lindern, M.; et al. (1992). "Translocation t(6;9) in acute non-lymphocytic leukaemia results in the formation of a DEK-CAN fusion gene". Bailliere's Clinical Haematology. 5 (4): 857–879. doi:10.1016/s0950-3536(11)80049-1. ISSN 0950-3536. PMID 1308167.
- ↑ 5.0 5.1 Sandahl, Julie Damgaard; et al. (2014). "t(6;9)(p22;q34)/DEK-NUP214-rearranged pediatric myeloid leukemia: an international study of 62 patients". Haematologica. 99 (5): 865–872. doi:10.3324/haematol.2013.098517. ISSN 1592-8721. PMC 4008104. PMID 24441146.
- ↑ Slovak, M. L.; et al. (2006). "A retrospective study of 69 patients with t(6;9)(p23;q34) AML emphasizes the need for a prospective, multicenter initiative for rare 'poor prognosis' myeloid malignancies". Leukemia. 20 (7): 1295–1297. doi:10.1038/sj.leu.2404233. ISSN 0887-6924. PMID 16628187.
- ↑ Ishiyama, K.; et al. (2012). "Allogeneic hematopoietic stem cell transplantation for acute myeloid leukemia with t(6;9)(p23;q34) dramatically improves the patient prognosis: a matched-pair analysis". Leukemia. 26 (3): 461–464. doi:10.1038/leu.2011.229. ISSN 1476-5551. PMID 21869835.
- ↑ Ageberg, Malin; et al. (2008). "Identification of a novel and myeloid specific role of the leukemia-associated fusion protein DEK-NUP214 leading to increased protein synthesis". Genes, Chromosomes & Cancer. 47 (4): 276–287. doi:10.1002/gcc.20531. ISSN 1098-2264. PMID 18181180.
Notes
*Primary authors will typically be those that initially create and complete the content of a page. If a subsequent user modifies the content and feels the effort put forth is of high enough significance to warrant listing in the authorship section, please contact the Associate Editor or other CCGA representative. When pages have a major update, the new author will be acknowledged at the beginning of the page, and those who contributed previously will be acknowledged below as a prior author.
Prior Author(s):
*Citation of this Page: “Acute myeloid leukaemia with DEK::NUP214 fusion”. Compendium of Cancer Genome Aberrations (CCGA), Cancer Genomics Consortium (CGC), updated 05/17/2025, https://ccga.io/index.php/HAEM5:Acute_myeloid_leukaemia_with_DEK::NUP214_fusion.